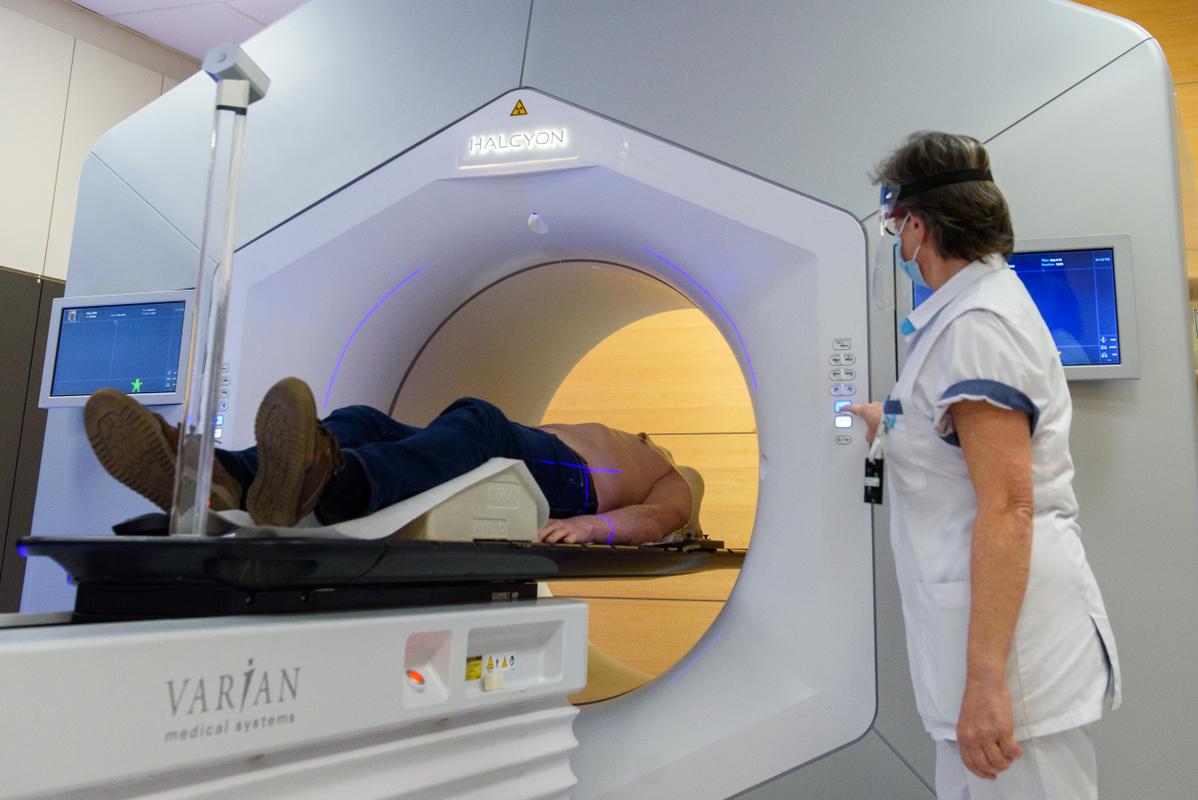
Even though radiotherapy is a common treatment for various types of cancer, such as prostate cancer, the use of preventive radiotherapy of the lymph nodes in the pelvis is still debatable. No scientific trial could prove that such radiotherapy could increase the chance of definitively curing the cancer. This changed recently: a group of international prostate cancer experts were able to show that high-risk patients do benefit from this. This multidisciplinary group was led by experts from UZ Leuven: professor Gert De Meerleer, doctor Charlien Berghen and professor Steven Joniau.
Risk threshold for metastases
Radiotherapist-oncologists denote the risk that a prostate tumour metastasises to the pelvic lymph nodes with a percentage between 0 and 100. De Meerleer and his colleagues concluded that prostate cancer patients with a risk factor of over 35 per cent would strongly benefit from whole pelvic radiotherapy.
The fact that cancer experts did not see the benefit of pelvic radiotherapy for such a long time, stems from a less favourable target group selection rather than the nature of the treatment, prof. dr. De Meerleer explains. “Trials conducted in France and the USA showed that preventive radiotherapy of the pelvis was hardly beneficial for patients with a low risk percentage. However, it is best to assist anyone that surpasses the risk threshold of 35 per cent – a selection we're making based on the PDA protein in the blood and the degree of aggressivenes of the tumour – with preventive pelvis radiotherapy, combined with 24 months of hormone therapy.”
Target group selection
De Meerleer and some ten radiotherapist-oncologist, medical oncologist and urologists shared their findings in a trial recently published in The Lancet Oncology. In it, they've assessed the results of all large international trials on pelvic radiotherapy for prostate tumours between 2014 and 2021.
De Meerleer: “Preventive pelvic radiotherapy significantly increases the chance of a definitive cure and a higher survival rate in patients with prostate cancer. It is however important to include the whole nymph node chain in the radation field and not just limit it to the nymph node regions deep in the pelvis. Modern radiation techniques, available everywhere in Belgium, limit the chance of developing serious adverse effects.”
Proton therapy
Since early this year, UZ Leuven has applied the new insights from the trial to their treatment of prostate cancer. In addition, the researchers hope that they will be able to implement proton therapy to radiate these high-risk patients. “It is important to achieve a radiation dose in the tumour that is high enough, while radiation of the healthy surrounding tissue should be kept as low as possible to protect the tissue maximally. Proton therapy allows us to fire targeted energy parts to a to-be-determined depth in the body, where they emit their energy and then stop. In the case of classic photon therapy, the radiation dose spreads further. Proton therapy is more expensive, but can also actively help prevent adverse effects in high risk prostate cancer. That is our conviction, which we want to strengthen through further research, to show the government the added value and to receive financial support, so that we can use proton therapy as a standard for this type of treatment in the near future”, according to De Meerleer.
Postponed care
Annually UZ Leuven treats more than five hundred prostate cancer patients. As a result of the coronacrisis and two lockdowns there is currently an increased influx. De Meerleer: “The past year and a half a lot of patients have postponed their consultation. You can guess the consequences: we're seeing more and more high-risk cases, on average 5 to 7 patients per month, which is significantly more than in the past. Our new insights, with better cure rates, could not have come at a better time.”