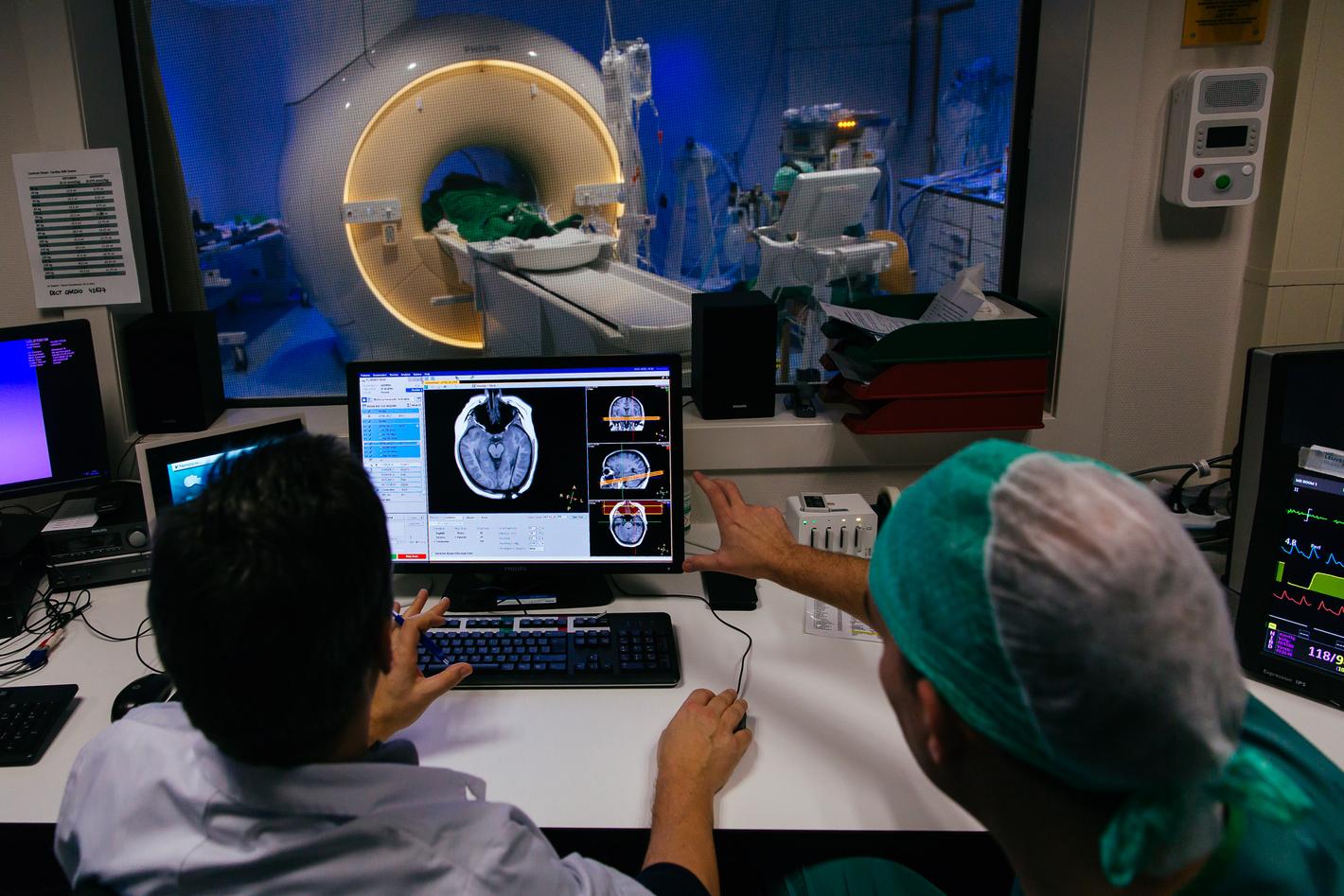
For one in three epilepsy patients medication only has a limited effect. If they also have regular epileptic seizures, they can qualify for epilepsy surgery. People with a lot of epileptic seizures find it very difficult to lead a normal social life. If the disorder cannot be controlled with medication, the neurosurgeon can decide to have brain surgery performed after an extensive pre-surgical evaluation. Tissue ablation via electrodes has been around for quite some time, but burning off the brain tissue that causes the epilepsy is less controlled. A new alternative is an ultra-thin laser in combination with a precise MRI as the GPS system.
The brain surgeon will drill a miniscule hole in the skull, after which a narrow tube is introduced through the cerebral membrane and into the brain with at the end a laser attached to it. A CT-scan in the operating theatre checks whether the probe is placed at the exact location. The patient is subsequently transferred from the operating theatre to the MRI scanner, where the surgeon can calculate meticulously where he wants to ablate tissue and at what temperature via intelligent software. The probe is then gradually moved along the abnormal brain tissue. This allows the laser to do its work very meticulously and to burn off the brain tissue causing the epilepsy. The surgeon will see the real-time results on the screen.
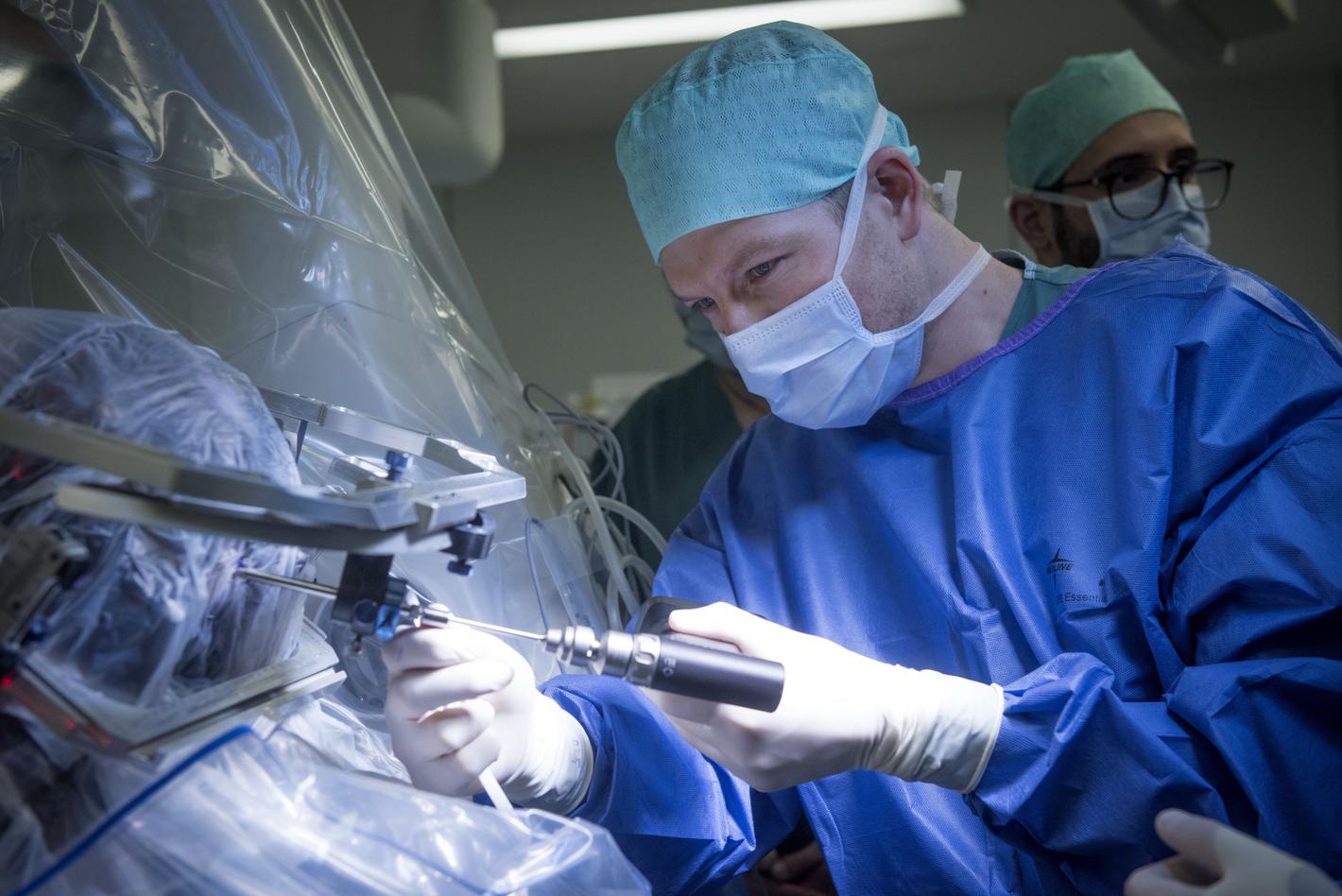
"An ultra thin laser with a precise MRI as a GPS system"prof. dr. Tom Theys
Ablation with laser precision
Burning off brain tissue holds risks. Because the procedure is carried out in an MRI scanner that monitors changes in temperature, the surgeon can see the temperature in the tissue he wants to ablate and in the surrounding area at all times. Certain nerve tracts surrounding the 'bad' brain tissue can be crucial for sight, reading, motor skills or speech. It is therefore very important to burn off the abnormal brain tissue in a controlled manner.
The tube that is introduced in the brain contains a cavity with water running through it to cool down the laser and to control the temperature very precisely. In comparison to a classic operation, the laser treatment takes less long and the treatment is also less strenuous for the patient. The patient's recovery time will also be lower than after classic brain surgery.
Delicate brain surgery
Because epilepsy is difficult to assess on a short term basis, physicians refrain from making statements about the long-term effects of the procedure. Fact is however that the UZ Leuven patient that underwent the surgery used to have several severe epileptic fits a day, and now, a month after the procedure, he's had only a few minor, non-troublesome fits.
Prof. dr. Tom Theys, neurosurgeon at UZ Leuven: “Such a type of laser treatment is delicate brain surgery, but the procedure was technically faultless. The abnormal brain tissue was burned off without having to damage the normal brain tissue. The fact that we can burn away the brain tissue in a controlled manner and in real time, is an important added value. It would be good to get together with other epilepsy centres to see how we in Belgium could offer this fairly expensive procedure to the limited number of patients who really need it.”
The new method is already being used in the US but now Europe will also be performing the procedure for a select group of epilepsy patients. The technique has also been used successfully worldwide for deep-lying brain tumours. As far as the cost to the patient goes, the operation is not yet covered by the conventional medical insurance RIZIV. In this case, UZ Leuven and the special solidarity fund contributed to the cost for the first patient. The procedure is a collaboration between the departments of neurology, anaesthesiology, radiology and neurosurgery.